BLOG

Updates Before Opening
We would like to take a moment to say thank you again for your loyalty and support. These have been incredibly trying days for our community but finally it seems that we can see a light at the end of the tunnel. Our team has been working hard to increase safety measures and protocols so…

Announcement – Melrose Family Dentistry & Bedford VA Hospital
We are happy to announce that we are now the exclusive dentist for the Bedford VA Hospital staff and families.

End Of Year Dental Insurance Reminder
We hope this letter finds you well and enjoying a pleasant fall. As the end of the year is quickly approaching, we want to remind you to utilize any unused insurance benefits before they expire. Many of you also participate in Flexible Spending Accounts or Health Savings Plans with your employer. In most cases, any…
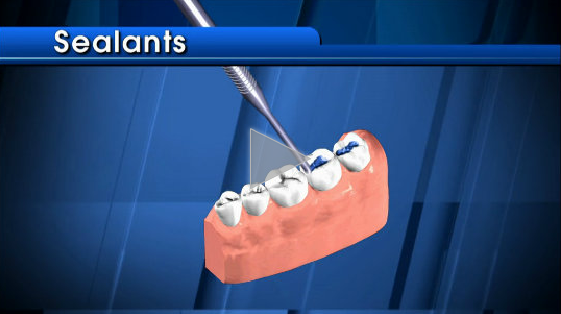
The Importance of Dental Sealants
Dental sealants act as a barrier to prevent cavities. They are a plastic material usually applied to the chewing surfaces of the back teeth (premolars and molars) where decay occurs most often. Thorough brushing and flossing help remove food particles and plaque from smooth surfaces of teeth. But toothbrush bristles cannot reach all the way…
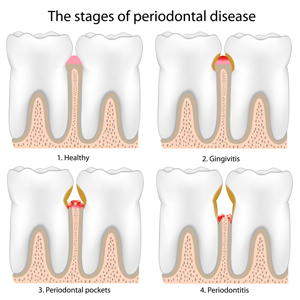
The Stages Of Periodontal Disease
What is periodontal disease? Periodontal disease, commonly referred to as gum disease, is an inflammatory disease that destroys the gums and other supporting structures around the teeth. Periodontitis (gum disease) is not to be confused with gingivitis (gum inflammation). Gingivitis usually precedes periodontitis. However, it is important to know that not all gingivitis progresses to…

Flossing, The Bad Breath Killer!
Need another reason to floss your teeth at least once a day? Flossing daily helps improve bad breath by effectively removing the food particles and bacteria that contribute to it. That makes flossing one of the easiest ways to prevent and banish bad breath. Bad breath, also known as halitosis, is more common than many…
Study Finds Energy, Sports Drinks Damage Tooth Enamel
Energy and sports drinks can damage tooth enamel, boosting the risk of cavities, according to a new study. “The big misconception is that energy drinks and sports drinks are healthier than soda for oral health,” says researcher Poonam Jain, BDS, MPH, associate professor and director of community dentistry at the Southern Illinois University School of…
New Study Suggests Dental Cleaning Reduces Risk Of Cardiovascular Diseases
A study observed more than 100,000 people, none of whom had a history of heart attack or stroke at the beginning of the study, over a period of seven years in Taiwan. The study suggested that those people who got their teeth professionally cleaned at least twice or more in two years had significantly lower…
Gum Disease Bacteria May Hamper Immune System
University of Pennsylvania researchers made a new discovery about the impact of periodontitis. Periodontitis often causes dysbiosis, which is a two-fold manipulation of the human immune system that diminishes the immune system’s effectiveness. The information appears in the journal Cell Host & Microbe. The periodontal bacterium Porphyromonas gingivalis impacts two pathways while eliminating immune cells…


